What is the Exposome? According to the CDC/NIOSH[1] website, the exposome can be defined as: “the measure of all the exposures of an individual in a lifetime and how those exposures relate to health. An individual’s exposure begins before birth and includes insults from environmental and occupational sources. Understanding how exposures from our environment, diet, lifestyle, etc. interact with our own unique characteristics such as genetics, physiology, and epigenetics impact our health is how the exposome will be articulated.” [2] In other words, the exposome is the analysis of risk factors encompassing environmental exposures (chemicals, diet, stress, and physical factors), behaviors and genetic variations with overall corresponding biological responses. This relatively new concept and approach in epidemiological and biomedical research has stirred up some excitement among scientists, with many calling for more efforts to map the human exposome,[3] in order to safeguard future generations from the increasing number of chemical pollutants in our environment. In this blog, we discuss the main factors comprising the skin aging exposome and how they impact our personal care and skin health.
The Skin Aging Exposome
Skin aging is caused by a combination of two cumulative processes: (1) intrinsic aging and (2) extrinsic aging. The former is the normal genetic process that occurs over time, including body’s internal oxidation due to metabolic activities and oxygen consumption;[4] while the latter, or accelerated aging, is resulted from exposure to skin exposome factors (Figure 1). Extrinsic environmental factors, such as sunlight, pollution, and climate, can trigger biological processes that participate and accelerate skin aging. Self-induced factors, such as smoking, and lifestyle choices also play a role in potentiating skin aging.
Specifically, Krutmann et al.[5] have proposed the following environmental factors as part of the skin aging exposome: (1) solar radiation: ultraviolet radiation, visible light and infrared radiation, (2) air pollution (ozone and diesel exhaust), (3) tobacco smoke, (4) nutrition, (5) other miscellaneous factors, including lifestyle choices and use of cosmetic products. In fact, it is estimated as high as 80% of skin aging signs are caused by the exposome.[6], [7] It is important to note that skin exposome factors often act synergistically to accelerate the aging process. For instance, “photo-pollution”[8] is the exposome resulted from the synergistic combination of sunlight and pollution. In the following, we will briefly describe each skin aging exposome factor.
- Solar Radiation
Since ancient times, humans have tried various methods to shield the harmful solar radiation and protect skin against the adverse effects of the sun. In modern times, more sophisticated photoprotection products, i.e., sunscreen and/or daily skin care products, have been developed for the prevention of acute (e.g., sunburn) and chronic (e.g., skin cancer and photoaging) skin damage that may result from exposure to ultraviolet rays (UVB and UVA).
However, with recent advances in skin care research, we have learned that wavelengths beyond the ultraviolet spectrum (UVB, 290–320 nm, and UVA, 320–400 nm), visible light (400–770 nm) and infrared (IR) radiation (770 nm–1 mm), contribute to skin damage in general and photoaging including pigmentary problems of human skin (Figure 2).[9] Consequently, attempts have been made to develop sunscreen and skin care products that not only protect against UVB or UVA radiation but also provide photoprotection against visible light and infrared radiations.[10]
1.1 Ultraviolet (UV) Radiation
The role of UV radiation in skin aging is well established and the term “photoaging” is coined to emphasize this cause-and-effect relationship. This is the most studied exposome factor in skin aging for the past several decades. Herein we will summarize a few key points from review articles on the role of UV radiations in skin aging:[11],[12],[13],[14]
-
- Exposure to UV radiation is the primary factor of extrinsic skin aging. It affects all three layers of the skin, e., the epidermis, dermis and hypodermis. This is the primary cause of early, premature wrinkles, sagging skin and pigmentation.
- All UV wavelengths (UVB, UVA2 and UVA1) rays contribute to photoaging of human skin.
- Susceptibility is strongly influenced by endogenous protection systems in human skin, such as skin pigmentation, DNA repair, antioxidant defense, etc.
- Acute stress responses and chronic damage responses drive the skin aging process.
- Photoaging mainly results from daily exposure to non-extreme, low doses radiation. UVA rays, in particularly long wavelength UVA1 is a major contributor.
- Lastly and most importantly, it is highly probable that the regular use of sunscreens can help delay the photoaging process of human skin.
1.2 Visible Light (VL)
Of even lesser energy, visible light (400–700 nm) accounts for approximately 50% of the total solar spectrum. It penetrates deeply into biological tissues and about 20% reaches the hypodermis. Evidence suggests that VL plays a fundamental role in hyperpigmentation, particularly in individuals with deeper skin phototypes (Fitzpatrick skin type III-VI) where persistent pigment darkening has been observed following VL exposure.[15], [16] It is demonstrated that the lower wavelength, higher energy portion of visible light (blue-violet light from 400 to 500 nm) is responsible for the highest pigmentation induced by VL. Even the green part of VL accounts for more than 30% of skin pigmentation.[17] Studies have shown that physiological doses comparable to 90 – 150 min of midday summer sun exposure can induce lasting pigmentation.16 Recently, a unique mechanism involving activation of melanogenesis via the opsin 3 photoreceptor has been described.[18]
1.3 Infrared (IR) Radiation
IR rays accounts for approximately 45% of the total solar energy received. Only the shortest wavelengths, IR-A (770-1400 nm) have sufficient energy for skin penetration to cause significant damage. IR radiation is known to upregulate the production of matrix metalloproteinases (MMPs), enzymes that facilitate the degradation of extracellular matrix proteins.[19] The earliest biological event that occurs after IR-A radiation in human fibroblasts is an increase in the intra-mitochondrial production of reactive oxygen species (ROS). There is a shift in the glutathione equilibrium to its oxidized state. The discovery of this mitochondrial signaling response caused by IR-A has a direct clinical impact as it indicates that the use of antioxidants may be an effective strategy to help protect the skin against effects from IR-A.
- Air Pollution and Tobacco Smoking
Exposures to pollutants, exhaust, smog-derived ozone and cigarette smoke have been associated with accelerated skin ageing (pigmentation, loss of elasticity and wrinkles) and increased cancer risks.[20] Airborne particles (particulate matters, PM), rich in polycyclic aromatic hydrocarbons (PAHs), can exert detrimental effects on human skin and contribute to facial lentigines formation.[21] In general, topical exposure to pollutants harms the skin by increasing oxidative stress that modifies lipid DNA and protein function.[22], [23], [24] Soeur and coworkers at L’Oréal demonstrated the effect of “photo-pollution”, where with exposure to UVA1 irradiation (i.e., long UVA, 350-400 nm), which accounts for 80% of daily UV and can easily reach dermal-epidermal junction in skin, air pollutants (in particular, PAHs) were phototoxic even at very low concentrations (nanomolar range) on cultured cells or in reconstructed epidermis. Thus, the impact of PAHs reacting to long UVA synergistically increases the oxidative stress, which may impair cutaneous homeostasis and aggravate sunlight-induced skin damage.
Exposure to pollution also decreases skin quality and exacerbates existing skin conditions, such as atopic dermatitis (AD) and acne.[25] Various scientific studies show an undeniable link between air pollution (including cigarette smoke) and pigmentation, loss of elasticity and wrinkles. These factors share a common mechanism involving the aryl hydrocarbon receptor (AhR).[26] Based on available studies, many of the adverse effects caused by air pollution may be mediated via AhR signaling in human skin. In addition to topical exposure, humans are exposed to PAHs via systemic accumulation in the body. This is evident by measuring the pollutants in the hair fibers.[27] Naudin et al. have confirmed that speed of naturally occurring hair-cortex degradation and cuticle delamination is increased in fibers with increased PAH concentrations. Further, hair fiber with exposure to UV irradiation leads to more pronounced cuticle damage, especially around samples with higher PAH concentrations. This detrimental effect of PAHs together with UV irradiation, i.e., photo-pollution, is likely to be seen with other human tissues.
- Diet / Nutrient
Dietary factors and nutritional supplements may influence skin health. Eating unhealthy food has been associated with numerous skin problems, ranging from acne to signs of skin aging. On the other hand, a healthy diet rich in antioxidants may delay chronological aging effects. In a study of facial aging in twins, twins who avoid excessive alcohol intake have a younger perceived age.[28] Consuming too much sugar is suggested to contribute to wrinkles, due to a natural process, known as glycation,[29] where sugar in the blood stream binds to proteins to form harmful molecules called “advanced glycation end products” (AGEs), aka. the Maillard reaction. Another risk factor associated with food consumption is unintentional ingestion of PAHs. In addition to inhalation and skin contact of PAHs as a result of air pollution, people can be exposed to PAHs by consuming charbroiled foods (smoke meat, or grilled over charcoal, diesel exhausts, etc.).[30] Such consumption may contribute to skin damages following systemic exposures.
- Stress and Sleep Deprivation
It is known that stress creates elevated levels of cortisol hormones which cause inflammation in the body. Inflammation leads to increased collagen breakdown and exacerbation of skin conditions such as acne, rosacea, eczema and wound healing. Though it may seem intuitive to link physiological stress and skin aging, the underlying mechanisms are not well defined. However, one plausible mechanism was demonstrated by studies of the correlation between psychological stress and permeability barrier homeostasis in human cutaneous functions, thus explaining how psychological stress can lead to a decline in epidermal permeability and deterioration in barrier disruption and recovery, followed by the induction, exacerbation, and propagation of inflammatory skin disorders. [31], [32]
Further to acute psychosocial stress, sleep deprivation is associated with increased signs of intrinsic skin aging (fine lines, uneven pigmentation, reduced elasticity), most likely due to its disruption of skin barrier function homeostasis, and that this disruption may lead to much slower recovery rates after skin barrier disruption and lower satisfaction with appearance.[33]
Exposome and Acne
Acne is caused by inflammation of the pilosebaceous follicle, occurring commonly in adolescents and some adults. Clinically, inflammatory acne causes skin damages and formation of skin lesions, including micro-comedones, papules, and pustules. In some people, scarring from acne can be persistent.[34]
Several exposome factors, including diet, pollution, medication, microbiota, and cosmetics, have been implicated in development and exacerbation of acne (Figure 3).23 This argument is confirmed in a recent international survey with 11,000 participants, aged between 15 and 39 years, with clinically confirmed acne or without acne. Consumption of dairy products, sweets, alcohol or whey proteins, as well as exposure to pollution, stress, certain mechanical factors and humid or hot weather or sun exposure, were significantly (all P ≤ 0.05) more frequently reported for the acne group than for the control group.[35] Some topical skincare and makeup products containing essential oils, powders, and alkaline skin cleansers and soaps have been associated with acne.23 Use of mild cleansers on a regular basis to keep the skin surface free of oil, dirt and debris can help prevent acne.
Maskne
For decades in some Asian countries, people regularly wear face masks to reduce the inhalation of pollution-related particles. It has nowadays taken another facet, i.e., to limit the spread of harmful viruses such as COVID-19. However, the negative impact of repetitive and prolonged mask wearing may cause “maskne” or mask-related acne and other skin issues, including breakouts, clogged pores, redness, itchiness and imperfections. Maskne is essentially a subset of acne mechanica, due to friction/rubbing from the mask, causing local pressure on the sweat glands and irritation of the skin barrier.[36], [37] Further exacerbation is induced by increased temperature and trapped moisture in the mask area due to the continuous use of face masks. No studies to date have evaluated “maskne”, however, current data suggests maskne is likely a result of local temperature changes and skin microflora dysbiosis.[38] General advise for dealing with maskne includes: (1) avoid wearing makeup under the mask area, (2) use mild facial cleanser containing salicylic acid, (3) topical moisturizer to hydrate and maintain skin barrier functions, and (4) change masks regularly.
Taking on the Exposome
In a 2016 review article, Dr. Sainani summarized progress in exposome research, including Environment-Wide Association Studies and novel data collection techniques, as well as significant remaining challenges in collecting, analyzing, and interpreting exposome data. The article concludes with a call to adopt a “big science” approach akin to the Human Genome Project, with investments in improving measurement techniques, establishing public databases with agreed upon standards, and strong community leadership.[39]
In a recent JEADV paper, Appenzeller et al. studied hair samples from 204 women from two Chinese cities with different levels of pollution. The hair analysis, together with “omics” data (metabolomics, proteomics, genomics and microbiome), provided access to information for assessing chronic exposure to pollution (particularly, PAHs) and shed light on the molecular mechanisms of the combined effects of exposome factors, including solar radiation and other environmental exposure.[40]
Further to the study on hair samples, De Vecchi et al. have evaluated the impact of several environmental aggressors on human surfaces, using portable and wearable devices for monitoring exposome.[41] The work was carried out by two bicyclists wearing multiple sensors to capture the meteorological conditions by biking through urban areas in summer and in winter in Brazil. Correlated with GPS and monitoring data, all these results provide insights on how environmental stressors affect the quality of different hair types and body surface according to exposure routine. Additional study was designed to quantify environmental exposures during routine daily activities to provide quantitative metrics that inspire future studies on exposome and human health.[42]
Summary and Conclusions
Based on several reviewed articles, it is undeniable that most skin aging processes are affected by numerous different exposome factors. In order to mitigate the negative impacts of such factors, further development of the nascent holistic approach will be important for the cosmetic field. In particular, a comprehensive approach is essential to understanding how the sum of all factors are affecting skin health and skin aging on the individual level and how to further define the appropriate recommendations, such as lifestyle changes, nutritional adjustments, adequate cosmetic formulations, and personalized beauty routine, to alleviate the negative impacts of such factors. While exposome factors cannot be completely avoided, a conscious awareness, limited exposure and healthy lifestyle can help reduce their negative effects on skin health.
Acknowledgement
The authors are most grateful to Luc Aguilar for his review and suggestions for the manuscript. In addition, we would like to thank the kind review and comments from Giorgio Dell’Acqua, Ronni Weinkauf, Jean-Baptiste Galey, Gustavo Luengo, and the L’Oréal Reading Committee.
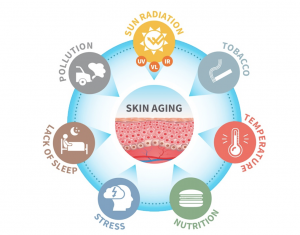
Figure 1. The skin aging exposome. These factors have been identified to have detrimental effects on skin health. Exposure to sunlight, pollution and tobacco smoking are shown to trigger molecular processes that damage the skin structure, leading to premature skin aging. Other factors, recently recognized and thus less studied, have also shown to be potentiators for skin aging. These factors can act independently or interact synergistically with each other to accelerate the skin aging process. [J. Krutmann, et al., The Skin Aging Exposome, J Dermatol Sci (2017)].
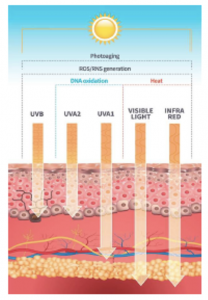
Figure 2. The solar spectrum with various wavelengths, which penetrate skin at different levels. The longer the wavelengths the deeper the rays penetrate the skin. Each wavelength has both different and overlapping effects. UV = Ultraviolet radiation, ROS = Reactive Oxygen Species, RNS = Reactive Nitrogen Species. [Modified from J. Krutmann, et al., The Skin Aging Exposome, J Dermatol Sci (2017) with updated data from H. Lim publications].
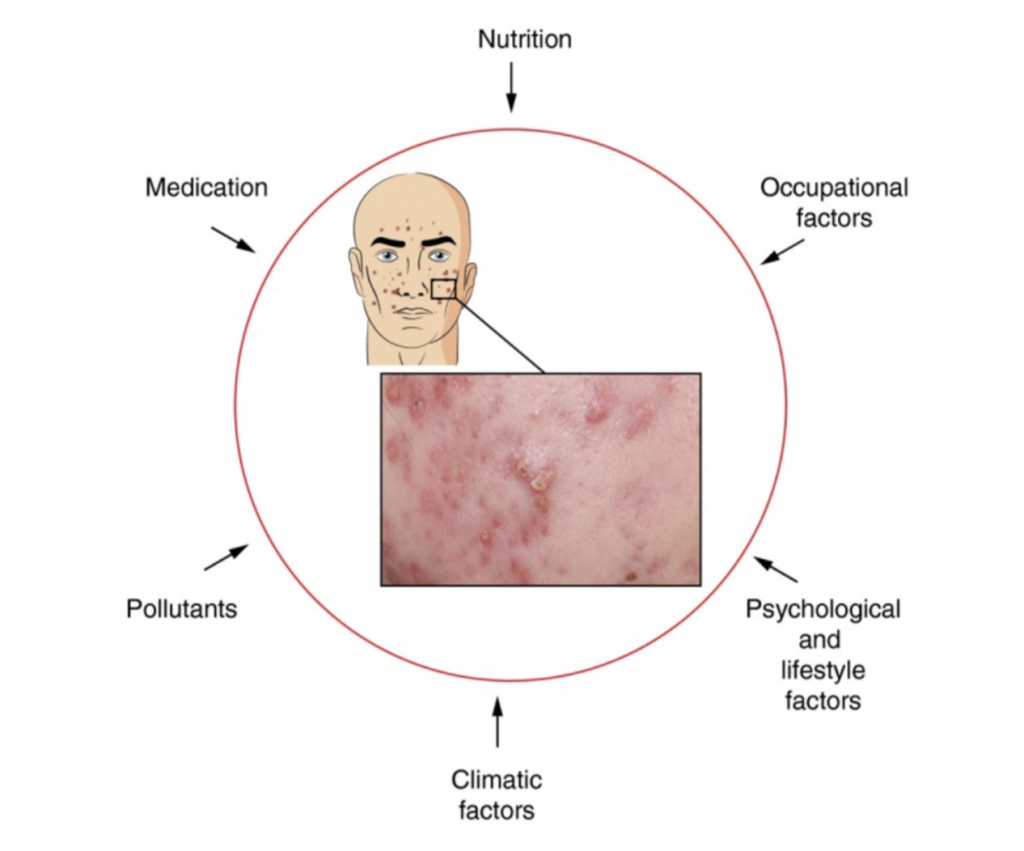
Figure 3. The exposome factors impacting acne. [B. Dreno, et al., J Eur Acad Dermatol Venereol, (2018)]
References:
[1] CDC = Centers for Disease Control and Prevention, NIOSH = National Institute for Occupational Safety and Health.
[2]https://www.cdc.gov/niosh/topics/exposome/default.html#:~:text=The%20exposome%20can%20be%20defined,from%20environmental%20and%20occupational%20sources (Accessed on April 1, 2021)
[3] http://alliance.nautil.us/article/242/mapping-the-human-exposome (Accessed on April 4, 2021)
[4] Van Beek, J.H.G.M., Kirkwood, T.B.L., Bassingthwaighte, J.B. ‘Understanding the physiology of the ageing individual: computational modelling of changes in metabolism and endurance’, Interface Focus.06 April 2016. http://doi.org/10.1098/rsfs.2015.0079
[5] Krutmann, J., Bouloc, A., Sore, G., Bernard, B.A., Passeron, T. ‘The skin aging exposome’, J Dermatol Sci. 2017 Mar; 85(3):152-161. doi: 10.1016/j.jdermsci.2016.09.015.
[6] https://www.vichyusa.com/vichy-exposome (Accessed on April 6, 2021)
[7] Friedman, O., ‘Changes associated with the aging face’, Facial Plast Surg Clin North Am. 2005 Aug; 13(3):371-80.
[8] Soeur, J., Belaïdi, J.P., Chollet, C., Denat, L., Dimitrov, A., Jones, C., Perez, P., Zanini, M., Zobiri, O., Mezzache, S., Erdmann, D., Lereaux, G., Eilstein, J., Marrot, L. ‘Photo-pollution stress in skin: Traces of pollutants (PAH and particulate matter) impair redox homeostasis in keratinocytes exposed to UVA1’. J Dermatol Sci. 2017 May;86(2):162-169. doi: 10.1016/j.jdermsci.2017.01.007. Epub 2017 Jan 16. PMID: 28153538.
[9] Note that IR rays do not trigger pigmentation. See Geisler, A.N., Austin, E., Nguyen, J., Hamzavi, I., Jagdeo, J., Lim, H.W. ‘Visible light. Part II: Photoprotection against visible and ultraviolet light’, J American Academy of Dermatol, Volume 84, issue 5 (May 2021).
[10] Dupont, E., Gomez, J., Bilodeau, D. ‘Beyond UV radiation: a skin under challenge’, Int J Cosmet Sci. 2013 Jun;35(3):224-32. doi: 10.1111/ics.12036. Epub 2013 Feb 14. PMID: 23406155.
[11] Marionnet, C., Tricaud, C., Bernerd, F. ‘Exposure to non-extreme solar UV daylight: spectral characterization, effects on skin and photoprotection’, Int J Mol Sci, 2014, 16: 68-90
[12] Battie, C., Jitsukawa, S., Bernerd, F., Del Bino, S., Marionnet, C., Verschoore, M. ‘New insights in photoaging, UVA induced damage and skin types’, Exp Dermatol, 2014, 23 Suppl 1: 7-12.
[13] Kligman, L. H., Kligman, A.M., ‘The nature of photoaging: its prevention and repair’, Photodermatol, 1986, 3: 215-27.
[14] Flament, F., Bazin, R., Laquieze, S., Rubert, V., Simonpietri, E., Piot, B., ‘Effect of the sun on visible clinical signs of aging in Caucasian skin’, Clin Cosmet Investig Dermatol, 2013, 6: 221-32
[15] Mahmoud, B.H., Ruvolo, E., Hexsel, C.L., Liu, Y., Owen, M.R., Kollias, N., Lim, H.W., Hamzavi, I.H. ‘Impact of Long-Wavelength UVA and Visible Light on Melanocompetent Skin’, J Invest Dermatol. 2010, 130: 2092-97.
[16] Duteil, L., Cardot-Leccia, N., Queille-Roussel, C., Maubert, Y., Harmelin, Y., Boukari, F., Ambrosetti, D., Lacour, J.P., Passeron, T. ‘Differences in visible light-induced pigmentation according to wavelengths: a clinical and histological study in comparison with UVB exposure’, Pigment Cell Melanoma Res. 2014, Sep.; 27(5):822-6.
[17] Personal communication with L. Aguilar.
[18] Regazzetti, C., Sormani, L., Debayle, D., Bernerd, F., Tulic, M.K., De Donatis, G.M., et al. ‘Melanocytes sense blue light and regulate pigmentation through the Opsin-3’, J Invest Dermatol. 2018, 138:171–8
[19] Vierkotter, A., Krutmann, J. ‘Environmental influences on skin aging and ethnic-specific manifestations’, Dermatoendocrinol, 2012 4: 227-31.
[20] Drakaki, E., Dessinioti, C., Antoniou, C.V. ‘Air pollution and the skin’, Front. Environ. Sci., 15 May 2014, doi.org/10.3389/fenvs.2014.00011
[21] Vierkötter, A., Schikowski, T., Ranft, U., Sugiri D., Matsui, M., Krämer U., Krutmann J. ‘Airborne particle exposure and extrinsic skin aging’, J Invest Dermatol. 2010 Dec;130(12):2719-26.
[22] Marrot, L. ‘Pollution and Sun Exposure: A Deleterious Synergy. Mechanisms and Opportunities for Skin Protection’, Curr Med Chem, 2018, 25: 5469-86.
[23] Dreno, B., Bettoli, V., Araviiskaia, E., Sanchez Viera, M., Bouloc, A. ‘The influence of exposome on acne’, J Eur Acad Dermatol Venereol, 2018, 32: 812-19.
[24] Lefebvre, M. A., Pham, D.M., Boussouira, B., Bernard, D., Camus, C., Nguyen, Q.L. ‘Evaluation of the impact of urban pollution on the quality of skin: a multicentre study in Mexico’, Int J Cosmet Sci, 2015, 37: 329-38.
[25] Lefebvre, M. A., Pham, D.M., Boussouira, B., Qiu, H., Ye, C., Long, X., Chen, R., Gu, W., Laurent, A., Nguyen, Q.L., ‘Consequences of urban pollution upon skin status. A controlled study in Shanghai area’, Int J Cosmet Sci, 2016, 38: 217-23.
[26] Abel, J., Haarmann-Stemmann, T. An introduction to the molecular basics of aryl hydrocarbon receptor biology. Biol. Chem. 2010, 391, 1235-1248.
[27] Naudin, G., Bastien, P., Mezzache, S., Trehu, E., Bourokba, N., Appenzeller, B.M.R., Soeur, J., Bornschlögl, T. ‘Human pollution exposure correlates with accelerated ultrastructural degradation of hair fibers’, Proceedings of the National Academy of Sciences Sep 2019, 116 (37) 18410-18415; DOI: 10.1073/pnas.1904082116
[28] Rowe, D.J., Guyuron, B., ‘Environmental and genetic factors in facial aging in twins’, in: Textbook of Aging Skin (Farage, M. A., Miller, K. W. and Maibach, H. I., eds.) pp. 441–446. Springer Berlin, Heidelberg (2010).
[29] Draelos, Z.D., Pugliese, P.T. ‘Glycation and skin aging: a review’, Cosmet. Toiletries Sci. Appl. 2011, 126 (6) 438.
[30] Hokkanen, M., Luhtasela, U., Kostamo, P., Ritvanen, T., Peltonen, K., & Jestoi, M. ‘Critical Effects of Smoking Parameters on the Levels of Polycyclic Aromatic Hydrocarbons in Traditionally Smoked Fish and Meat Products in Finland’. Journal of Chemistry, 2018. https://doi.org/10.1155/2018/2160958
[31] Garg, A., Chren, M.M., Sands, L.P., Matsui, M.S., Marenus, K.D., Feingold, K.R., Elias, P.M. ‘Psychological stress perturbs epidermal permeability barrier homeostasis: implications for the pathogenesis of stress- associated skin disorders’. Arch Dermatol. 2001 Jan;137(1):53-9.
[32] Altemus, M., Rao, B., Dhabhar, F.S., Ding, W., Granstein, R.D. ‘Stress-induced changes in skin barrier function in healthy women’. J Invest Dermatol. 2001 Aug;117(2):309-17.
[33] Walia, H.K., Mehra, R. ‘Overview of Common Sleep Disorders and Intersection with Dermatologic Conditions’, Int J Mol Sci. 2016 Apr 30;17(5):654. doi: 10.3390/ijms17050654.
[34] Ramasamy, S., Barnard, E., Dawson, Jr., T.L., Li, H., ‘The role of the skin microbiota in acne pathophysiology’, Br J Dermatol, 2019, 181: 691-9.
[35] Dreno, B., Shourick, J., Kerob, D., Bouloc, A., Taïeb, C. ‘The role of exposome in acne: results from an international patient survey’, J Eur Acad Dermatol Venereol. 2020 May; 34(5):1057-1064.
[36] Sinha, A. & Singh, A. R. ‘An Unforeseen Hazard of Masks Being in Vogue’. Int. J. Occup. Environ. Med. 2020, 11, 213–214.
[37] Teo, W. ‘The “Maskne” microbiome – pathophysiology and therapeutics’. Int. J. Dermatol. 2021, doi:10.1111/ijd.15425.
[38] Searle, T., Ali, F. R., Al-Niaimi, F. ‘Identifying and addressing “Maskne” in clinical practice’. Dermatol. Ther. 2020, 8–9. doi:10.1111/dth.14589.
[39] Sainani, K.’ Taking on the Exposome: Bringing Bioinformatics Tools to the Environmental Side of the Health Equation’. Biomedical Computation Review November 1st (2016).
[40] Appenzeller, B.M.R., Chadeau-Hyam, M., Aguilar, L. ‘Skin exposome science in practice: current evidence on hair biomonitoring and future perspectives’’, JEADV 2020, 34 (Suppl. 4), 26-30.
[41] De Vecchi, R., da Silveira Carvalho Ripper, J., Roy, D., Breton L., Germano Marciano, A., Bernardo de Souza, P.M., de Paula Corrêa, M. ‘Using wearable devices for assessing the impacts of hair exposome in Brazil’. Sci Rep. 2019 Sep 16;9(1):13357. doi: 10.1038/s41598-019-49902-7. PMID: 31527774; PMCID: PMC6746720.
[42] De Paula Corrêa, M., Germano Marciano, A., Silveira Barreto Carvalho, V., Bernardo de Souza, P.M., da Silveira Carvalho Ripper, J., Breton, L., Roy, D., De Vecchi, R. ‘Exposome extrinsic factors in the tropics: the need for skin protection beyond solar UV radiation’, Science of The Total Environment, 2021, 146921, ISSN 0048-9697.
AUTHORS
Catherine CHIOU,a Gabrielle SORE,b Stephen LYNCHa
a L’Oréal Research and Innovation, Clark, NJ, USA
b L’Oréal Research and Innovation, Chevilly Larue, France

Catherine Chiou, PhD.
Dr. Catherine Chiou holds a BS degree in Chemistry from National Taiwan University and a Ph.D. in Bioinorganic Chemistry from the University of Minnesota. Catherine’s NIH Postdoctoral fellowship training in Synthetic Chemistry took place at Harvard University. Her first industrial position was with Unilever Research US in the laundry bleach research program and machine dishwashing detergent research, including I&I applications.
Catherine began her career in cosmetic field at L’Oréal USA in 2001 in the DIMP (International Raw Materials Department). She worked on all aspects of “innovative raw material” functions, including scouting new supplier innovations, and managing supplier relationships. In addition, Catherine served a stint within the PCPC INCI Committee.
Catherine is currently an Associate Principal Scientist at L’Oréal USA in the Cosmetic Application Domain, focusing on developing skin cleansing and makeup removing technologies. Prior to the current position, she has worked in the skin care research and innovation lab as a senior formulator, contributing towards development of platform technologies and several global launches of skin care treatment products. She is an inventor for more than 20 US and international patents. She is a current member of scientific committee of NYSCC.

Gabrielle Sore, PhD.
Dr. Gabrielle Sore is a pharmacist with a Ph.D. in dermal pharmacology. She has been working for more than 30 years in the cosmetic industry. Dr. Sore spent the last 29 years in L’Oréal where she worked in France, in Japan, and in the United States. During Gabrielle’s career, she worked mostly in the scientific communication of skin care, make-up and specific eye products; and she was more specifically in charge of scientific communication of dermatological brands like Vichy, La Roche Posay, SkinCeuticals for which her role is to coordinate the information within the Research, Marketing and Development teams.

Stephen Lynch, PhD.
Dr. Stephen Lynch holds a PhD in organic chemistry and spent 10 years in the pharmaceutical industry conducting drug discovery research. For the past 7 years he has worked for L’Oréal USA Research & Innovation where he currently serves as Director of Skincare Scientific Affairs. In this capacity he helps to identify cosmetic ingredients, coordinate innovative testing, and translate scientific concepts in support of skincare product development.
