How Many Languages Does our Skin Speak? A fresh look at what it can it teach us in terms of innovation if we listen.
Inflammation is Just the Beginning:
Inflammation has garnished the attention of mainstream headlines for the past 20 years and has certainly taken center stage describing and managing the current virulence of the pandemic. With terms like cytokine storm, pre-existing conditions and co-morbidities, what have we learned and what we still need to learn to properly manage the ill effects of inflammation and its impact on health is astounding. As a biologist, I adopted the general tenant that inflammation is the root of all evil when it comes to aging and disease, particularly in the skin. Whether its role is in normal aging from a subclinical perspective or pathological in nature in an acute verses chronic situation, inflammation seems to be a rate limiting step or first domino to fall for most underlining causes of both intrinsic and extrinsic aging processes in our largest organ the skin. Even in the Covid-19 era, we are seeing persistent skin rashes documented post infection, why? What are we doing right and what should we be doing different?
The good news is that we seem to understand inflammation from a mechanistic point of view. How reactive oxygen, metals, lipid mediators, enzymes, transcription factors, temperature, microbes and sun play a role in skin inflammation is well documented. The disconnect here is that we in the industry of cosmetic science have decided to treat the sources of inflammation as individual events rather than a consortium of cumulative ever changing processes designed to mute our first line of defense. This is akin to putting a lock box around a fire alarm verses reducing existing fire hazards.
In this regard, let us not loose site of the purpose of inflammation, which is to alert and respond to acute threats to homeostasis or skin balance. Every level of our biological organization has its own cadence on how homeostasis is maintained and managed over time. From a molecular level, through soluble cytokines (the language of our cells) all the way to behavior responses, evolution has afforded us a great deal of redundancy in this regard, all culminating to the ultimate goal of maintaining health and balance. In what follows, I hope to serve up a fresh look at how we as skin care technology providers can approach new product designs and formulation innovations that not only address acute disturbances in skin but may ultimately change the way we look and feel about our skin and ourselves as a whole.
The Skin as a Sensory Organ:
The best part of focusing on the skin is that it does so much for us in terms of our survival, health, and our ability to adapt to the environments we find ourselves in on a daily basis. Furthermore, the epidermis and some of the cell types that reside in it (melanocytes, Langerhans-like phagocytes) are embryologically derived from ectoderm which also gives rise to our nervous system proper. This is a profoundly underappreciated opportunity as our skin has all of the “gear” needed to effectively communicate with the nervous system as well as the endocrine system and vice versa. In this regard, we need to integrate the fact that our neural, endocrine, immune, skin microbiome and skin biology are all interlaced and cross talk every moment of our existence. The ability of our skin to react to its environmental threats through inflammatory processes has opened a window into a world that is vastly more complex and interactive. It requires a master’s degree in linguistics to hear all the talk between keratinocytes, immune cells, hair follicles and sweat glands and melanocytes. As a result, this conceptual understanding opens up targets that not only affect the skin proper but our behavior as well. What if we could understand the autonomic picture our brain has of our skin? I believe we would see numerous snap shots of skin grafts unique to one another, painted by skin thickness, pH, lipid structure, water content, hair follicle density, immune residence and microbiome attendance. Could we re-focus our formulation efforts in terms of sensory to be more inclusive of these micro environments and their associated biology? Could we change the way our brain “sees” our skin?
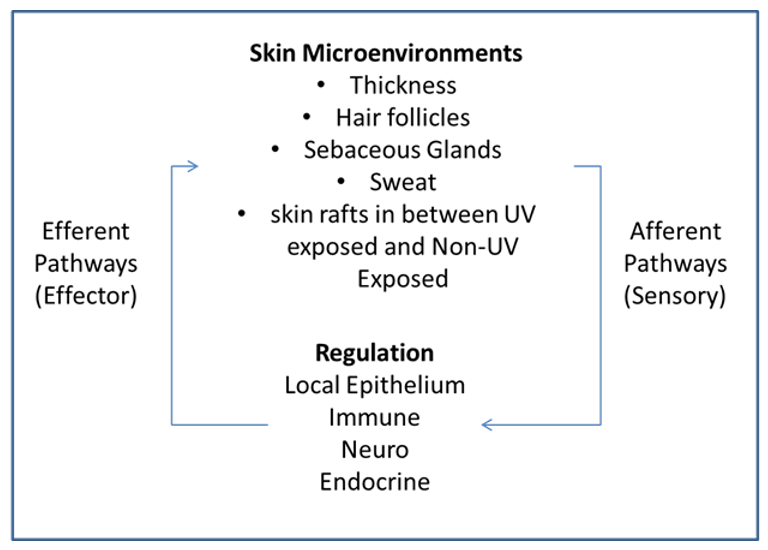
Behavior is driven by how we perceive our surroundings. Our skin is considered a neurosensory organ much the same way other species use antennae or chemoreceptors to “see” their environment as demonstrated by insects and snakes respectively. Our skin senses electromagnetic radiation, temperature, chemicals, pH, biological insults, and subtle changes in our microbiome. It also knows when there are sub clinical changes in chemistry as well as disruptions in barrier and wounding. All of these stimuli we cannot see with our other senses unless they are out of sync or control. We tend to focus more on sight and sound as an organism. Why then do we ignore the largest sense organ we possess when it has so much to say? More so, all of these stimuli are transmitted to the brain (consciously or unconsciously) and to the surrounding cells and tissues simultaneously, thus having an impact not only on our behavioral responses but on our epidermal biology, our immune and endocrine systems. Furthermore, the reverse is true. The brain and adrenals along with the immune cells talk back. A fundamental requirement for communication is that more than one entity needs to deliver information to another that can receive and react to it. How cool is it that whatever stimuli the skin observes it is translated via different systems that act in concert to maintain homeostasis and dictate behavior. As formulators and inventors, the next level of innovation will come from exploiting these lines of communication. Recall how simple the Wright brother’s solution to flight was compared to the latest version of air travel today. You will most likely not be in a position to imagine a jet airliner if you never saw the Kitty Hawk.
Immune System Integration:
If things were not complex enough, we need to consider the immune system and all of its abilities and functions as a driver of skin health. The marvelous thing about our immune system is that it is driven not just by genetics but also by environmental pressures we expose our body to on a regular basis. The immune system adapts and learns and has a periodicity that is defined by age and time. Our immune functions start out naive then grow, mature, plateau and decline throughout our lifespan. Furthermore, our immune system is organized into two systems (innate and adaptive/learned) that together synergize in function. It even has its own residential lymphoid cells called skin associated lymphatic tissue or SALT which supervises and coordinates your interactions with all things non-self. From that organization it specializes in various modalities of responses that are classified into 3 groups depending on the type of initiation involved and cytokine profile released into the milieu along with contributions from epithelial cell derived cytokine signals such as IL-33. For example Type I immunity is relegated to intracellular threats (viruses and parasites) and the production of IFN-g and/or TNFα. Type 2 immune responses are in ordinance with itch and are caused by harmful substances driven by the secretion of IL-4, IL-5 and IL-13. Type 3 immunity is specific to extracellular bacterial and fungal infections and characterized by the production of IL-17 and IL-22 cytokines. It is interesting to note that the cytokine profiles of each type of immunity dictate a specific ordered response by immune tissue, but they also modulate sensory perception and behavior, another key component to our overall host defense arsenal. For example, IL-33 release from keratinocytes in a compromised epidermal barrier can stimulate local neurons to become hypersensitive and hyper-excitable, thus releasing neuropeptides like substance P and CGRP, which then feedback on the very same keratinocytes to increase their proliferation in an effort to restore the compromised barrier. As a result, the hypertrophy can further disrupt epidermal differentiation, trap bacteria and acne and/or folliculitis ensues respectively in affected sebaceous gland canals and hair follicles respectively. Furthermore, antibodies to IL-13 and IL-4 (type 2 immune responses) reduce barrier inflammation which reduces itch in AD stuffer’s.
By grouping immune type cytokine profiles together along with their temporal expression patterns that includes initiation, plateau and resolution makes for a more precise technology development strategy in this regard.
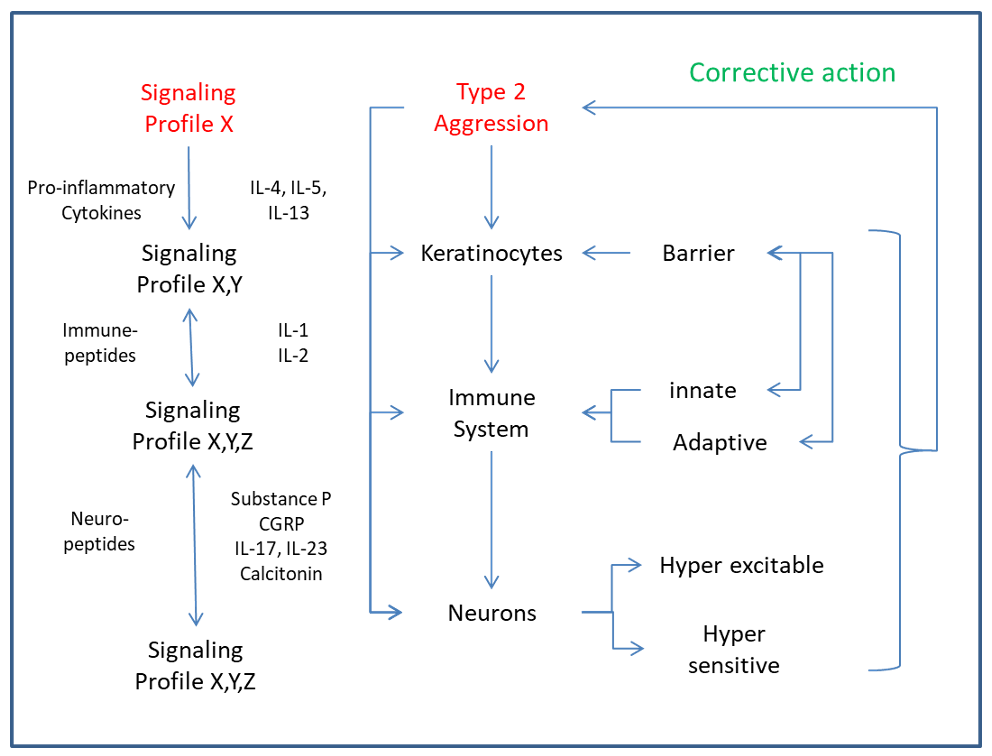
A Systems Approach to Understanding:
It is an interesting to note that the nervous system and its functions rely on afferent signals (sensory neurons and their associated stimuli) to understand its place in the environment, whereas the immune system also “senses” our body’s interactions with our surrounding through more of a military surveillance strategy of touch, chemical codes, catabolism and synthesis. Furthermore, the brain and its neurons are fixed in place converting chemical signals into electrical and back again at supersonic speed whereas the immune system is both static and dynamic adapting and learning at a significantly slower pace alongside the brain. It evolves and grows. The interplay between both of these systems tends to out rank the local tissue signals in which they reside. A linear approach to skin therapy has focused primarily on the residential populations of the skin with a peripheral mention of the other systems as secondary is like only listening to one side of the conversation. Leveraging a systems approach to new skin therapeutics and personal care technologies could lead to significant transformational innovations in product development including new categories of skin care.
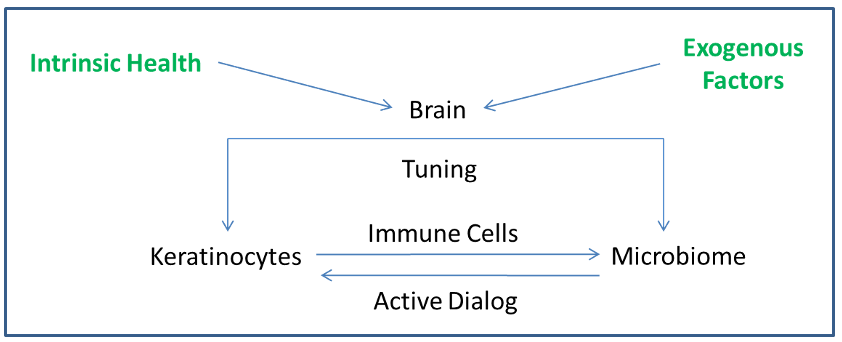
How does all of this work and where are we headed?
Advances in sensory biology (specifically itch and pain) have elucidated novel mechanisms that arose from our understanding of inflammation. Itch and pain are great examples of behavior changes as we have all experienced both. What if by understanding how to modulate these behaviors we could apply these same strategies to resolve dry skin, alter tone and texture, improve radiance and create the de-novo synthesis of endogenous beneficial molecules such as vitamin D, melanin and keratin. Furthermore, what if we could take these strategies forward to build better nails and hair, modulate sebum quality and quantity and even provide some level of subconscious behavior that could help you lose weight, reduce stress or just be happier? We spend a lot of time and energy trying to reduce acne which has significant behavior ramifications especially in teenagers, when in actuality, if we could just reduce the erythema in a timely manner, most of the terrible downstream problems would be better tolerated or ameliorated such as post inflammatory hyperpigmentation and self-esteem related syndromes.
Melanocyte Biology Reimagined:
Since melanocytes are the focal point of Post Inflammatory Hyperpigmentation, they could be considered the “conductor” of the cross talk between residential skin cells, neurons and immune processes. These cells that act as a UV detectors in our skin may in actuality have the ability to sense and focus on other stimuli. They are of course derived from the same primordial soup as neurons. If true, these master regulators would need to communicate with and receive signals from all cell types including neurons, macrophages, Langerhans cells and various lymphoid tissues (SALT). Just like neurons, melanocytes convert energy to communicate. Here melanocytes convert electromagnetic energy (UV and HEV) into relevant biological signals that initiate signal amplification and recruitment of multiple tissues to ultimately elicit a behavior change. The same signaling molecules that have a role in the central and peripheral nervous tissue also have a role in cutaneous melanocytes. These include signaling pathways that include Wnt, bone morphogenetic proteins, endothelins, hepatocyte growth factor, fibroblast growth factors, and neurotrophins.
Applying the Concepts:
When afferent sensory neurons fire in our skin, they release neuropeptides in an efferent (reciprocal) manner that has its effects on melanocytes and immune cells simultaneously. In other words, the skin is already reacting to the stimuli before the brain even gets the signal. This is an important event as this profile of cellular signals creates a customized code of signals unique to the stimuli, very similar to the basic formula for how your brain remembers a memory. If by understanding this profiling technic our body uses on the local level we could indeed teach our skin to react in different ways by nudging and modulating profile dynamics.
This concept is already in practice through the use of antibody therapy for psoriasis and atopic dermatitis (AD). These antibody therapies work by interfering with the cytokine-induced pathways in neurons, important for intercellular conversations with local cytokines which then in turn modulates itch and inflammation. The immune therapeutic Tofacitinib works through JAK inhibition thus reducing inflammation better than traditional broad spectrum anti-inflammatory strategies (systemic steroids). Here the traditional modality of treating the source of the problem is over ridden by muting the signal that helps propagate it. Additionally, this neuron targeted approach is also supported by the observations that patients with inflammatory (AD) experienced resolution of inflammation in body parts that experience nerve loss. What are we to conclude from this? Chronic inflammation requires communication with the nervous system.
Integration of the Skin Microbiome:
Peeling back yet another layer of the onion, we need to include our newfound tribe the skin microbiome. In collaboration with the gut microbiome, these two tribes have considerable influence on everyday life as it relates to well-being and health. If you wonder of their overall purpose, it lies in their ability to adjust tolerance and direct the necessary “activation energy” needed to amplify inflammation, over and above the status quo. Think of it as immune exercise or conditioning. The diversity of microbes in and on our body translates and cross-trains all the different biological conversations between the skin epithelia, immune cells and processes along with the existing neural architecture. The “chatter” establishes a level of readiness. It results in an overall host defense that is primed and semi-activated to address danger and invasion. When microbiome diversity is lowered or dominated by a few select species, the response is detrimental by two-fold. One, it allows for re-colonization of the skin by opportunistic invaders which may not be pathological at normal levels but create that cytokine profile or “storm” that trips the balance of cross talk between all the players resulting in an increase in entropy of the whole system. Chaos, isn’t that what we all work so hard to control? Two, the low diversity establishes a lower state of readiness and as result the conversations become quieter and limited leaving the health of the skin vulnerable to imbalance and thus, putting negative pressure on behavior. Can we blame our little friends for our actions and thoughts? Absolutely! Just as folks with AD, psoriasis, irritable bowel syndrome and Crohn’s disease.
In closing:
As a result of all this biological chatter we have order and purpose. It is exciting to see how fundamental understanding evolves. The integration of multiple languages into a new one with higher purpose, efficiency and meaning is an evolutionary learning process. To naively think we understand the language of our biological complexity is limiting our potential. We must integrate and transcend across the mechanistic understanding and incorporate a multi-disciplinary approach to new concepts and ideas. We need to explore new ways to achieve desired responses and ultimately behavior that favors well-being for all ages and health both physically and mentally. I can’t help but wonder how many times we find ourselves enjoying a good meal, listening to our favorite music or being with friends and family that creates a sense of well-being that is most grounded. Isn’t that what you would like to have in a product? These feelings can’t be solely due to cerebral contentment, you have billions of other contributing opinions looking out for the same sense of well-being. It’s time to listen more intently to those conversations. One could have a hard time arguing which system truly dominates the conversation and thus our behavior and as a result our health. Let not your strategy and ideation be limited to just one language.
Inspiration was gleaned from the following references:
The Neuro-Immune Axis in skin Sensation, Inflammation and Immunity, Anna M. Trier et. al., J Immunol, 2019 May 15: 202(10): 2829-2835.
Melanocytes: A Window into the Nervous System, Mina Yaar, et. al. Journal of Investigative Dermatology Volume 132, Issue 3, Part 2, March 2012, Pages 835-845
Inflammatory Resolution: New Opportunities for Drug Discovery, Derek W. Gilroy, et. al., Nature Reviews /Drug Discovery May 2004, 401-416.

Michael Anthonavage
VP of Operations & Technology
Eurofins CRL Cosmetic Testing, Inc.
Michael Anthonavage has 20+ years of experience in personal care product development and a career spanning background in skin biology. Michael has extensive knowledge in product development and product design. He specializes in R&D to marketing translation, including claims validation both in-vitro and in-vivo. He is an engaging public speaker and product technology advocate with an ability to marry complex ideas and concepts to various consumer needs. Michael is currently the VP of Operations & Technology at Eurofins CRL Cosmetic Testing, INC. Michael’s previous positions have involved R&D leadership positions at Johnson & Johnson Consumer Products, Presperse and Vantage Specialty Chemicals. Michael is currently on the NYSCC Scientific Advisory Board and has won a variety of industry awards for his contributions in research and product development. He has a number publications and patents to his name and continues to be an influential speaker in the personal care, bioinstrumentation and skin testing arena.
